Modernize and streamline data exchange
Ensure ongoing compliance and deliver a better member experience with our award-winning interoperability platform.
Achieve complete and accurate risk capture to enhance care quality and outcomes
Complete and accurate risk capture is essential to success in value-based contracts. Effective risk adjustment can improve revenue accuracy, enhance care quality, and reduce compliance and audit risks—but achieving this is often easier said than done. Combing through mountains of clinical data requires time and resources that many provider organizations simply don’t have at their disposal.
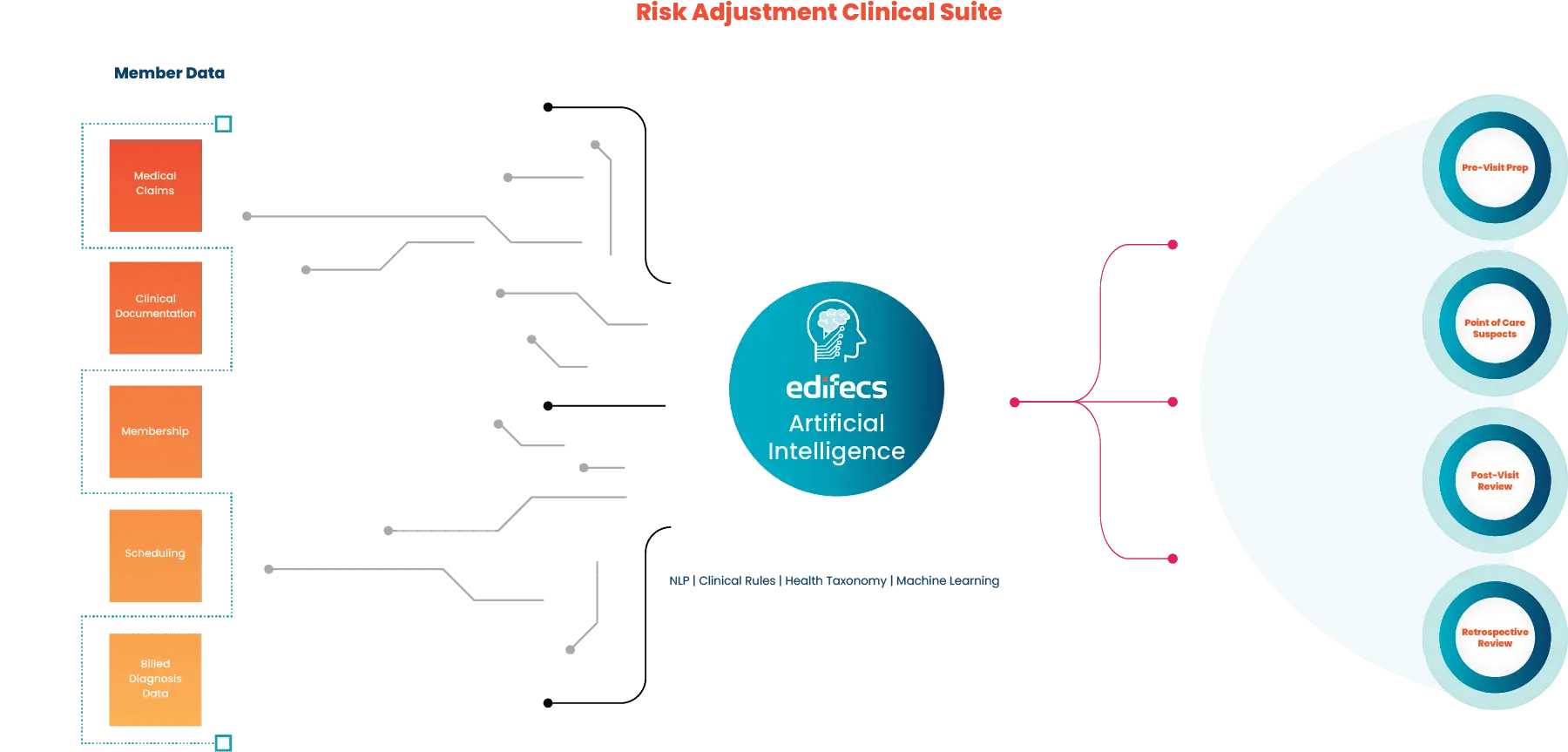
The Risk Adjustment Clinical Suite is a SaaS-based, modular solution that seamlessly integrates with EHRs to augment—not undermine—existing clinical workflows. Using AI-derived insights and our proprietary Natural Language Processing (NLP) engine, the Clinical Suite enables provider organizations to simultaneously achieve complete and accurate risk capture for multiple patient populations.
Ensure ongoing compliance and deliver a better member experience with our award-winning interoperability platform.


Pre-Visit Prep
Point of Care Suspects
Post-Visit Review
Retrospective Review
By delivering better satisfaction, better clinical outcomes, and better population health, value-based care can transform healthcare. Effective risk adjustment is essential to success in value-based care—but for many provider organizations, achieving complete and accurate risk capture is easier said than done.
How much is a properly coded Hierarchical Condition Category (HCC) code worth?
The specific value of a single HCC code varies according to the rate set by CMS and the risk scoring methodology in use (e.g., CDPS, CDPS+Rx, or D-SNP, depending on the state); however, gaps in HCC coding can cause up to a 12% loss in annual revenue for healthcare providers.
How are RAF scores calculated?
Numerical weight is assigned to a patient’s demographic factors (age, sex, race, ZIP code, residence, disability status, socioeconomic status, Medicaid eligibility, and institutional status) and to the HCC codes in their chart; the values of the HCC codes are measured cumulatively.
These numbers are added together to calculate the Risk Adjustment Factor (RAF) score. The RAF score is then multiplied by the CMS rate for each individual HCC to calculate the expected annual cost of care.
What is the most common reason for improper payment?
According to a 2022 HHS report, insufficient documentation was responsible for an astonishing 91.7% of improper payments by CMS:
| Reason for Improper Payment | Frequency |
|---|---|
| Insufficient, inadequate, or missing documentation | 81.2% |
| Incorrect coding | 10.5% |
| Other | 8.3% |